News
Stronger DVA Claims Start With the Right Medicals

Navigating the DVA claims process can be overwhelming, especially when it comes to understanding medical evidence. If you're unsure where to start or what reports you need, you're not alone. At Front Foot Health, we support veterans by providing the medical assessments they need to build stronger, clearer, and more successful claims.
Here’s everything you need to know.
What Are DVA Medical Assessments?
Medical reports are an important part of your DVA claim. These reports indicate how your health condition is connected to your time in service. They help DVA understand how service life has affected your physical or mental health, and they’re a critical part of making sure you receive the entitlements and support you deserve.
Common Mistakes That Can Affect Your DVA Claim
Many veterans face similar challenges when submitting their claims. Some of the most common issues include:
- Incomplete forms or missing details, which can cause delays or result in the claim being denied.
- Inconsistencies between documents, such as differing details from various providers or across reports, which can raise questions.
- Lack of a clear link between the condition and service, making it harder for DVA to recognise the condition as service-related.
Working with a provider who understands the process can help you avoid these pitfalls and submit a stronger, more complete claim.
Why Choosing the Right DVA Medical Provider Matters
DVA medical reports aren’t like standard GP reports. They require specific information, correct formatting, and clear links to your service history. That’s why it’s essential to work with a provider who understands the DVA process inside and out.
A provider who specialises in DVA medical assessments can offer more than just appointments. They help strengthen your claim in several key ways:
- They carefully review your documentation to ensure it meets DVA requirements, reducing the risk of delays or rejections due to errors or missing information.
- They present medical evidence clearly and effectively, making it easier for DVA to assess and process your claim.
- They may identify additional conditions linked to your service that you didn’t realise were eligible for support.
- They can also assist with completing related DVA forms, ensuring everything is submitted correctly and on time.
How Front Foot Health Supports Veterans
Front Foot Health is a veteran-led organisation that specialises in DVA medical assessments. Our team has clinicians and staff with personal and professional experience in the veteran space, with many of us being veterans ourselves or from veteran families.
Here’s how we support you:
- Veteran-led care: We understand the DVA system and the lived experience of service.
- Fast-tracking the process: Access our network of GPs and specialists (including dermatologists, gastroenterologists, endocrinologists and more) to reduce long wait times.
- Dedicated admin contact: You’ll have a clear point of contact throughout the process. No confusion, and no chasing multiple people for updates.
- Flexible access: Choose from in-person or telehealth consults, available Australia-wide.
- Ongoing support: Whether you have an advocate or not, we can guide you on what assessments you need and when.
When Should You Organise Your DVA Medicals?
It depends on each case. We recommend reaching out to our team and discussing your specific situation for the best course of action.
If you’re working with an advocate, we’ll coordinate with them directly. If you’re not, our team can still walk you through the steps and help you get everything you need.
Ready to Take the Next Step?
Getting your medicals sorted is one of the strongest ways to set your DVA claim up for success. We’ll help guide you through the process with experience, empathy, and expert care.
Contact Front Foot Health: Australia’s veteran-focused provider for accurate, compliant, and fast DVA medical assessments.
DVA Inconsistencies
PROBLEM:
The Department of Veterans' Affairs (DVA) is saying one thing publicly and doing another in practice. They are denying their changes are adversely affecting veterans when the data proves otherwise. They are not engaging with providers, which is in direct contradiction to the Royal Commission into Veteran Suicide’s recommendations
WHAT IS HAPPENING:
At Senate Estimates (March 2026), DVA stated that:
- Veterans can choose their own medical providers
- Veterans are not required to use specific assessment providers
- Claims are progressing through the system
- DVA appears to have privately contracted Hearing Australia to perform assessments and veterans who have not used these clinics have ongoing pending determinations.
However, in frontline practice, we are seeing:
- Veterans being told their claims will not progress unless they use MLCOA
- DVA staff continue directing veterans to specific providers
- Data requested by the Senate on provider outcomes has not been supplied
- Current serving veterans are being told they must have assessments and reports completed by ADF Medical Officers or go to MLCOA. ADF does not have capacity to perform.
WHAT THIS MEANS FOR VETERANS:
- Veterans are given conflicting informaton
- Real choice of provider is limited
- Trust in the system is undermined
Veterans are being forced to navigate a system where rules are unclear, inconsistent and where veteran outcomes are not the priority.
WHY THIS MATTERS NOW:
- Nearly 100,000 claims are already in the system
- Over 100,000 additional claims are expected from July 2026
If the inconsistencies remain delays will increase, confusion will worsen and the system pressure will intensify. This will mean independent providers leave the sector, and veterans are left with no choice and limited medical advocates.
RECOMMENDATIONS:
- Hold DVA to account over their inconsistencies
- Ensure DVA has their own Senate Estimates hearing instead of following Defence
- Establish independent oversight to verify compliance
- Provide transparent data on provider use and outcomes
- Work with independent providers to strengthen their position instead of pushing them to leave the sector
The State of Veterans’ Affairs in Australia

A system failing those it was built to serve April 2026
Foreword
Dr Tim Nelson
Founder and CEO at Front Foot Health
As both a clinician and a veteran, I approach this system from two perspectives: as a provider of care, and as someone who has relied on it.
This report reflects a growing tension between clinical best practice and system design.
Modern healthcare is built on principles of patient-centred care, continuity, and accessibility. These are not aspirational concepts — they are fundamental requirements for effective treatment, particularly in populations with complex and chronic conditions such as veterans.
The findings presented within this report suggest that, in several key areas, current policy settings are diverging from these principles.
Importantly, this report does not argue against reform. In fact, we are pushing for it. Veteran health systems must evolve.
However, the effectiveness of reform depends on how it is implemented — particularly the extent to which it incorporates the perspectives of those it affects.
The current approach to veteran healthcare and reform, led by the Department of Veterans Affairs, does not involve meaningful consultation with the veteran cohort or their treating practitioners.
Kneejerk policy changes, driven solely by budget considerations, are a sure way to even further restrict access to critical treatment for one of our most medically complex cohorts.
From a clinical standpoint, the themes emerging in this report — access barriers, administrative burden, constraints on treatment pathways, and lack of trust — warrant careful but immediate consideration. These factors have direct implications for patient outcomes.
This report provides a valuable evidence base to inform that discussion. It is our hope that this report will act as the voice of Australia’s veterans, as they speak out for more choice, better access, improved health supports, and a patient-driven system which not only understands their needs but prioritises them.
Executive Summary
A national survey of 1,141 Australian veterans was conducted in February 2026 and reveals a system under pressure and a veteran community that is increasingly losing confidence in it.
Key findings include:
- Trust in DVA sits at just 2.6 out of 10, with nearly 80% rating it 3 or lower
- 89% of veterans say they are not meaningfully consulted before major policy changes
- 94% believe they should choose their own healthcare providers 65% say they do not have genuine choice in how services are delivered
- Mental health is critically low, averaging 2.8 out of 10 42% say removing telehealth would disrupt their access to care
Taken together, these findings point to more than dissatisfaction.
They point to a system that veterans increasingly feel is being done to them, not with them.
What veterans are telling us
Mental health is at a critical low
Veterans report an average mental health rating of 2.8 out of 10.
At the same time, more than 40% say they cannot reliably access mental health support when they need it.
This is one of the most confronting findings in the report.
Low mental health scores at this level indicate a population experiencing significant psychological and psychiatric strain. When combined with inconsistent access to care, it raises serious questions about system responsiveness to one of the most critical areas of veteran health.
Given our country has conducted multiple parliamentary inquiries and investigations into how to lower veteran suicide rates, this finding should shock our entire government into immediate action.

A collapse in trust
Trust is the foundation of any healthcare system. Without it, even well designed services struggle to function effectively.
Right now, that foundation is weak.
Nearly four in five veterans rate their trust in DVA at 3 out of 10 or lower.
This reflects a sustained erosion of confidence in the institution responsible for delivering veteran care.
When trust falls to this level, it begins to influence behaviour — including whether veterans seek care, adhere to treatment or engage with the system at all.
4 in 5 veterans don't trust DVA

Rating it 3/10 or lower
Decisions made without them
Almost 9 in 10 veterans say they are not meaningfully consulted before major policy changes.
This points to a structural absence of stakeholder engagement in decision making processes.
Decisions affecting treatment pathways, access and eligibility are being made without the consistent input of those directly impacted.
Over time, this creates a disconnect between policy intent and lived experience and it is often in that gap where trust deteriorates most rapidly.
9 out of 10 not meaningfully consulted

Choice is being eroded
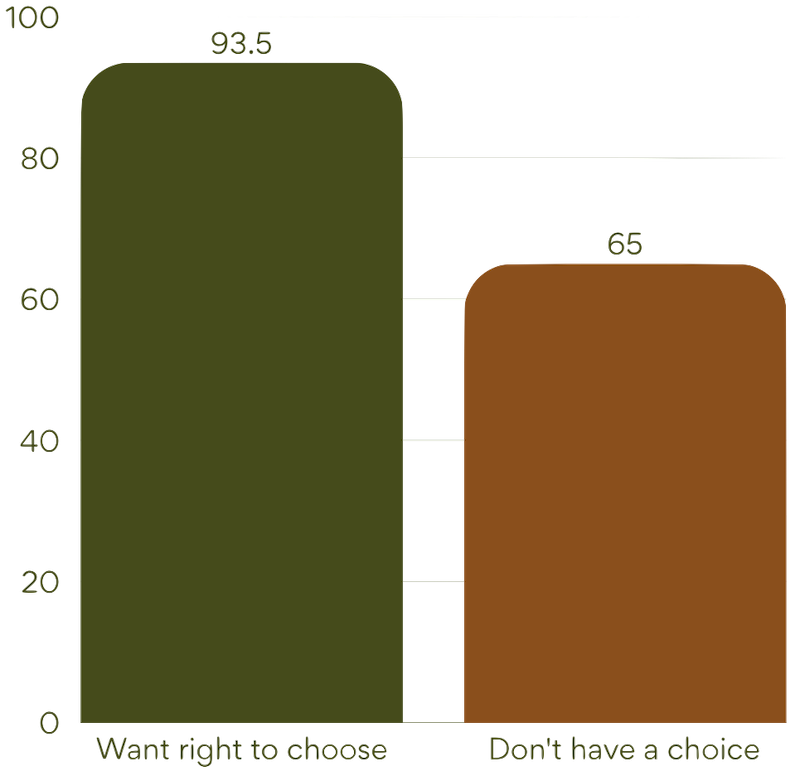
The message here is unequivocal:
- 93.5% want the right to choose their provider
- Yet 65% say they do not have genuine choice in practice
This gap between expectation and experience for our veteran cohort is significant.
Choice in healthcare is not simply about preference — it underpins continuity of care, therapeutic relationships and, most importantly, patient confidence. When veterans feel that choice is being constrained, it can lead to disengagement and fragmented care.
Changes brought in by the Department in February 2026 further reduce choice for veterans, and instead push them into a single provider model via the government’s tendered provider.
This not only removes veteran autonomy, but it further increases the lack of trust veterans have in the system.
The relationship between a veteran and their treating GP should be of utmost importance to the Department and the government, but current changes show it is not.
Access is getting harder
Nearly one in three veterans report delays accessing treatment, while many identify administrative burden and policy restrictions as key barriers.
This points to systemic friction within the way care is accessed and delivered by Australian veterans.
For a population with complex, often chronic conditions, delays and administrative complexity are more than inconveniences. They can often disrupt treatment continuity, exacerbate health conditions, increase reliance on acute care pathways, or result in the patient not seeking support at all.
Over time, these barriers accumulate and create a system that feels increasingly difficult to navigate and it often pushes veterans out completely, where many self-medicate or don’t receive treatment at all.
1 in 3 veterans delayed accessing treatment

What this means
Individually, each of these findings is concerning.
Together, they point to something more significant: a system experiencing cumulative pressure across trust, access and responsiveness.
This is not about a single policy decision or isolated failure. It is about a pattern:
- Decisions made without consultation
- Restrictions introduced without clear alignment to patient need
- Structural barriers that build over time rather than being resolved
The risk is not only declining satisfaction. It is gradual disengagement from the system itself.
And increasingly, that is what veterans are saying.
Recommendations
To rectify this concerning situation, the below recommendations should be implemented as a matter of government urgency.
-
Enshrine veteran choice of treating practitioner as a non negotiable principle across all DVA-funded care.
-
Establish a clear, consistent, and legislated definition of “treating practitioner” to prevent arbitrary exclusion.
-
Remove structural barriers that direct veterans toward DVA appointed providers over their chosen clinicians.
-
Ensure telehealth access is available on equal terms for all providers, not limited to government-contracted services.
-
Align fee schedules with true cost of service and ensure parity between DVA-appointed providers and independent clinicians.
-
Fund and reduce administrative burden on clinicians to prevent provider withdrawal from veteran care.
-
Guarantee access to clinically appropriate diagnostic investigations regardless of provider type.
-
Eliminate bottlenecks by allowing veterans to access assessments through their own practitioners rather than a single contracted provider.
-
Prohibit the overriding of clinical judgement by administrative processes, particularly in determining condition stability and treatment pathways.